Campylobacter: A leading foodborne pathogen
What is Campylobacter?
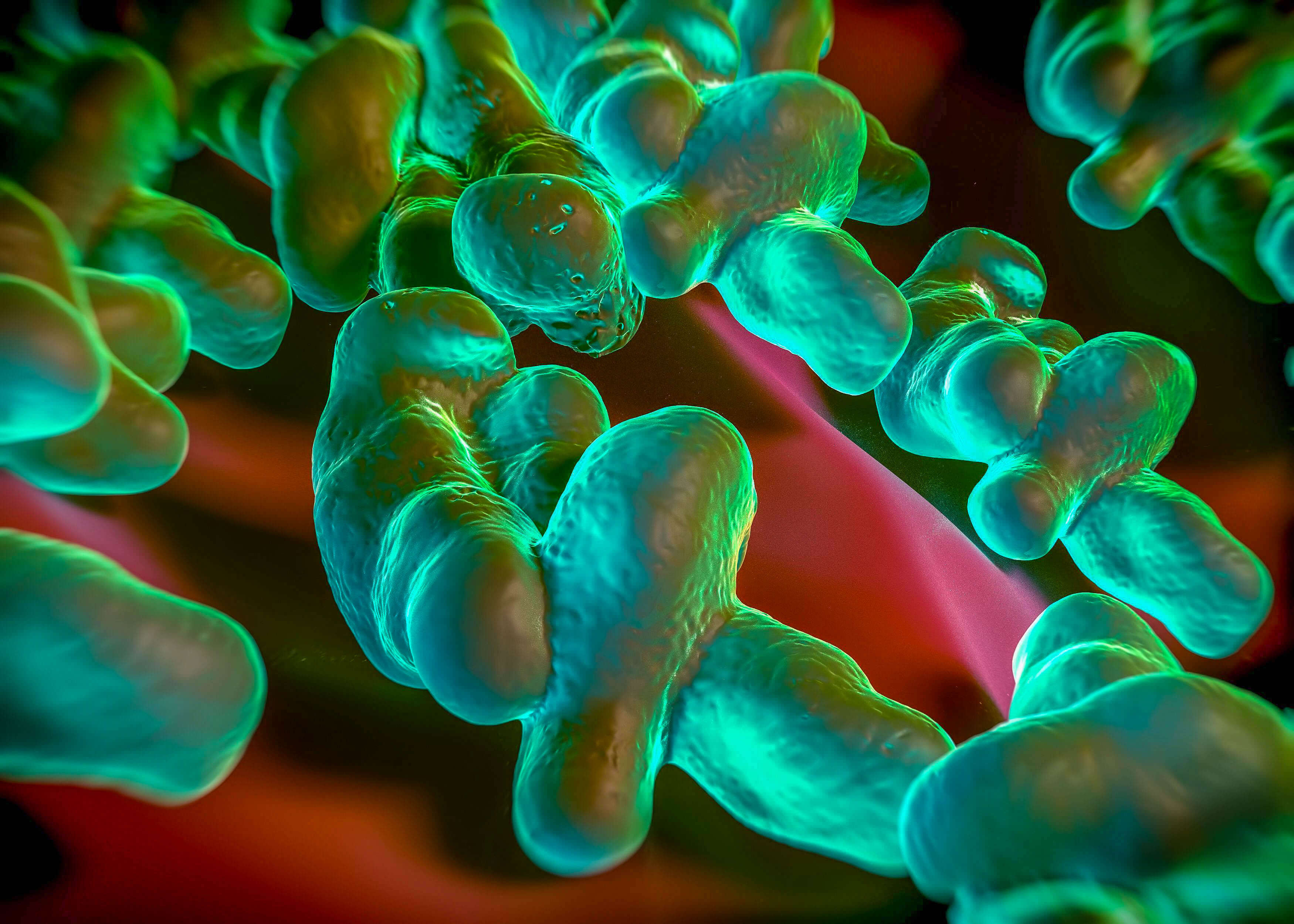
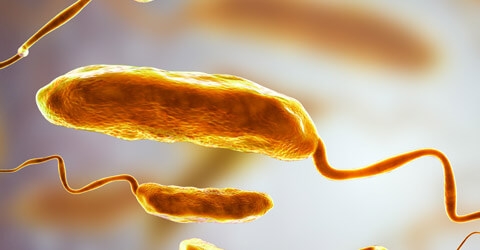
The Campylobacter, a genus of gram-negative and non-spore forming bacteria, belongs to the family of Campylobacteraceae and includes a total of 27 species1. Those are small curved-spiral bacilli, with a characteristic spiraled « corkscrew » motility. They are microaerophilic, capable to grow at 37°C and some of them, defined as thermotolerant Campylobacter, are also able to grow at 41.5°C.
Campylobacter is the most common bacterial cause of human gastroenteritis in the world and campylobacteriosis is the most commonly reported zoonosis.
Many chickens, cows, and other birds and animals that show no signs of illness carry Campylobacter.
Most human illness is caused by one species, called Campylobacter jejuni, but other species also can cause human illness.
What is the Campylobacter Associated Risks?
Campylobacter species are widely distributed in most warm-blooded animals.
They are prevalent in food animals such as poultry, cattle, pigs, sheep and ostriches; and in pets, including cats and dogs2. The bacteria have also been found in shellfish.
Campylobacter has a low infective dose (less than 500), which means that coming into contact with a few bacteria can cause illness. Patients infected with Campylobacter may experience mild to severe illness. Symptoms may include (bloody) diarrhoea, abdominal pain, fever, headache and nausea. The mean duration of illness is 2–5 days but can be up to 10 days. Infection can be associated with serious complications.
The most common are C. jejuni and C. coli and are responsible for gastroenteritis in humans.
The other emerging species such as C. consicus, C. upsaliensis, C. ureolyticus, C. hyointestinalis and C.sputorum have been associated with gastroenteritis and periodontitis. In some cases, infection of the gastrointestinal tract by these bacteria can progress to life-threatening extra-gastrointestinal diseases3, 4.
C. jejuni is also considered as one of the most common risk factors for developing Guillain-Barré syndrome (GBS), a rare autoimmune disorder in which a person’s own immune system damages the nerves, causing muscle weakness and sometimes paralysis and even fatality.
About 1 in every 1,000 reported Campylobacter illnesses leads to GBS and its symptoms may last for a few weeks to several years. Campylobacter infection leads up to 40% of GBS cases in the United States5.
It is often difficult to trace the sources of exposure to Campylobacter; this is due to the sporadic nature of the infection and the important role of cross-contamination. Campylobacteriosis remains a problematic disease to prevent and infection epidemiological trend continues to remain high throughout the world.
How Can the Presence of Campylobacter Be Detected?
The presence of Campylobacter in a ready to eat (RTE) food is considered potentially injurious to health.
Various internationally recognized methods (ISO standards) are used for the detection and enumeration of Campylobacter species, such as ISO 10272-1:2017 for detection and ISO 10272-2:2017 for enumeration6.
The enrichment culture methods uses Bolton Broth which allows resuscitation and recovery of injured organisms7 for accurate detection and enumeration. The traditional detection method gives presumptive results in 3 days, however for confirmed results, additional morphological, biochemical and growth tests are required which takes 3 days.
Various alternative diagnostic methods are currently used to save time and labour and have led to enhanced detection, identification and quantification of a broad range of Campylobacter species, such as immunological tests using antibodies can be used to capture the target antigen and fully automated Enzyme-linked Immuno-Sorbent Assay (ELISA) test and Polymerase chain reaction (PCR).
More recent and rapid identification method, MALDI-TOF MS (Matrix Assisted Laser Desorption Ionization-Time of Flight Mass Spectrometry identifies a microorganism based on its unique protein profile.
How can Campylobacter be prevented and controlled in the food industry
The food industry can prevent Campylobacter contamination by using a proactive approach and food safety standards, such as HACCP (Hazard Analysis Critical Control Point) and Environmental Monitoring Programs. (see our expert point of view on Environmental Monitoring Program)
Most of the regulatory requirements mandate the sampling of meat products for Campylobacter testing at different stages, such as in the raw and finished products.
Food manufacturing processes such as heating, freezing or chilling can cause sub-lethal injury to Campylobacter species, resulting in increased sensitivity to antibiotics and lower resistance to elevated temperatures.
Campylobacter contamination of raw poultry products occurs during slaughter operations, as well as during the live-animal rearing process (e.g., on-farm contamination can coat the exterior of the bird and remain attached to the skin). Contamination can be minimized with the use of proper sanitary dressing procedures.
To keep under control the contamination of carcases during the slaughtering process, a new process hygiene criterion for Campylobacter in broiler carcases is laid out in Regulation (EC) No. 2017/1495 since 1 January 2018,.
These control measure aims at reducing the prevalence in poultry farms.
What is The Treatment for Campylobacteriosis?
Most people with Campylobacter infection recover without specific treatment and treatment is not generally required, except electrolyte replacement and rehydration.
Patients should drink extra fluids as long as the diarrhea lasts.
Antibiotics are needed only for patients who are very ill or at high risk for severe disease, such as people with severely weakened immune systems.
However, the increasing drug resistance among different Campylobacter species pose a challenge for treatment of Campylobacteriosis.
Due to high occurrence of acquired ciprofloxacin resistance in Campylobacter however, this drug will not be effective for treatment of Campylobacter infections in many countries.
CDC estimates Campylobacter causes an estimated 1.3 million illnesses each year in the United States (2017)
Key Figures
- CDC estimates Campylobacter causes an estimated 1.3 million illnesses each year in the United States (2017). Most cases are not part of recognized outbreaks, and more cases occur in summer than in winter.
Data (sources): https://www.cdc.gov/campylobacter/index.html - In 2017, the number of reported confirmed cases of human campylobacteriosis in EU was 246,158. And the actual number of cases is believed to be around nine million each year.
Despite the high number of human campylobacteriosis cases, their severity in reported case fatality was low (0.04%), even though this was the third most common cause of mortality among the pathogens considered.
Data (sources): https://www.efsa.europa.eu/en/topics/topic/campylobacter
and EU summary report on zoonoses, zoonotic agents and food-borne outbreaks 2017 (EFSA Journal 2018;16(12):5500)
What Common Industries are Affected by Campylobacter?
The common industries affected by Campylobacter are food, agriculture and pharmaceutical.
These species pose a significant risk of zoonotic transmission due to their ability to colonize farm animals (cattle and pigs); companion animals (such as dogs and cats) and wild animals (birds such as ducks and gulls) and therefore can be found in many foods of animal origin
Campylobacter is also commonly present in all avian species fit for human consumption.
Campylobacter infections have been associated most often with poultry, raw (unpasteurized) dairy products, untreated water, and produce.
Poultry is a common source of infection. Eating undercooked chicken, or ready-to-eat foods that have been in contact with raw chicken, is the most common source of infection.
How is the Campylobacter Bacteria Transferred?
Campylobacter is responsible for zoonoses and the transmission occurs via the fecal-oral route through ingestion of contaminated food and water. The primary environmental niche is represented by the intestinal tract of all avian species, mainly poultry (i.e. broilers, laying hens, turkeys, ducks, and ostriches) which is considered the main route of transmission. The consumption of their meat, in fact, represents 50-70% of human cases of Campylobacteriosis. Even the consumption of raw milk, raw red meat, fruits, and vegetables, and shellfish8 has been identified as a possible cause of transmission of this disease.
BIOMÉRIEUX SOLUTIONS AND PRODUCTS
Sample and culture media preparation:
- DILUMAT® gravimetric diluter
- SMASHER® lab blender
- MASTERCLAVE® automated media preparator
Traditional Culture media:
Large range of traditional and standard culture media
Chromogenic culture media for alternative methods:
- CAMPYFOOD agar (CFA) Selective isolation and enumeration of Campylobacter from food and environmental samples
- CAMPYFOOD broth (CFB - MNB) Selective enrichment of Campylobacter from food and environmental samples
List of official validations: https://www.biomerieux-industry.com/products/culture-media-food-applications (bottom of the page)
Rapid enumeration solutions:
- TEMPO® CAM for the enumeration of Campylobacter
List of official validations: https://www.biomerieux-industry.com/products/tempo-food-quality-indicators (bottom of the page)
Rapid detection solutions:
VIDAS® Enzyme Linked Fluorescent Assay (ELFA) pathogen detection automated platform:
- VIDAS® CAM for the detection of Campylobacter
List of official validations for VIDAS® methods
https://www.biomerieux-industry.com/products/vidas-high-performance-food-pathogen-detection
(bottom of the page)
BIOBALL® - Standardized Strains for food applications:
- BIOBALL® A small freeze dried water-soluble Certified Reference Material containing a precise number of viable micro-organisms for your Microbiological Quality Controls
- BIOBALL® LUMINATE 2.0 Green Fluorescent Protein Strains (GFP), Genetically Modified Microorganisms (GMM) to distinguish from natural contaminants
Identification:
- API® galleries (large range)
- VITEK® 2C GN
- VITEK® MS
List of official validations https://www.biomerieux-industry.com/products/identification
(bottom of the page)
AST (Antibiotic Susceptibility Testing)
ETEST
Miscellaneous:
GENbox microaer
GENbag microaer
Combibag (consumable)
Campylobacter spp latex kit